Understanding and Navigating United Healthcare Prior Authorization: A User-Focused Guide
Navigating the United Healthcare prior authorization process can be frustrating, especially for first-time users who are unsure of where to start. The aim of this guide is to demystify the process and provide you with step-by-step guidance that addresses your pain points, offers practical solutions, and equips you with actionable tips to ensure smooth and timely approvals for your medical needs.
Prior authorization is a process where United Healthcare reviews medical treatments, procedures, pharmaceuticals, and services to determine if they will cover them under your health plan. This ensures that you only receive medically necessary care while controlling costs. If you find yourself needing to obtain prior authorization, this guide will help you understand the essentials and how to approach it effectively.
Quick Reference
Quick Reference
- Immediate Action Item: Verify if your service requires prior authorization by checking the United Healthcare website or contacting their customer service.
- Essential Tip: Fill out and submit the prior authorization form accurately and completely to avoid delays in approval.
- Common Mistake to Avoid: Missing or incorrect patient information can lead to rejections; double-check all data before submission.
Step-by-Step Guide to United Healthcare Prior Authorization
Let's delve into a comprehensive, easy-to-follow process to help you through the United Healthcare prior authorization procedure.
Step 1: Determine if Prior Authorization is Required
The first step in the prior authorization process is determining whether your service or medication needs prior authorization. To do this, follow these steps:
- Consult Your Health Plan Documentation: Review your United Healthcare member materials, including the Evidence of Coverage or Member Handbook. Look for a list of services that require prior authorization.
- Visit the United Healthcare Website: On the official United Healthcare website, you can find a list of services that may require prior authorization. This is also where you can access downloadable forms and useful resources.
- Contact United Healthcare Customer Service: If you're still unsure, you can reach out to United Healthcare's customer service for clarification. They are available to help you determine whether your specific service needs prior authorization.
Step 2: Gather Necessary Documentation
Once you’ve determined that prior authorization is required, you’ll need to gather all the necessary documentation. This usually includes:
- Provider Information: Have your healthcare provider ready with details such as their license number, contact information, and the nature of their practice.
- Patient Information: Collect your personal information, including your member ID number, date of birth, and contact information.
- Clinical Information: Prepare clinical details about the service or medication, including medical codes (e.g., ICD-10, CPT), and the diagnosis for which the service is being requested.
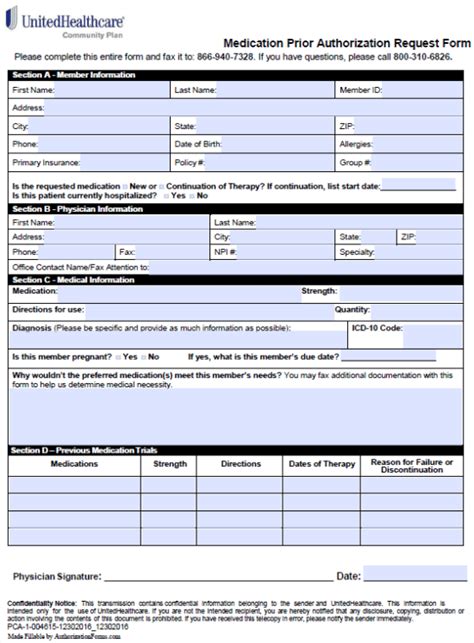
Step 3: Complete and Submit the Prior Authorization Form
Now, it’s time to fill out and submit the prior authorization form:
- Download the Form: Find the appropriate prior authorization form on the United Healthcare website or request it from your provider.
- Fill Out the Form: Ensure that you provide all required information accurately. Common sections to fill include patient details, service description, and provider information.
- Attach Supporting Documents: Include all the necessary clinical and patient information you gathered in Step 2.
- Submit the Form: Send the completed form and supporting documents to United Healthcare either by fax, mail, or through an online portal if available. Make sure to check the submission guidelines for the fastest processing time.
Step 4: Track Your Prior Authorization Request
After submitting your prior authorization request, it’s important to keep track of its status:
- Use Online Tools: United Healthcare provides an online tool where you can check the status of your request. This allows you to monitor progress without waiting for a call.
- Follow Up: If you haven't received a decision within the expected timeframe, don't hesitate to follow up with United Healthcare’s customer service. They can provide updates on your request.
Step 5: Receive and Act on the Decision
Once United Healthcare reviews your request, you will receive a decision. Here’s how to proceed based on their decision:
- Approved: If the request is approved, you’ll receive confirmation. Proceed with the service or medication as scheduled.
- Denied: If your request is denied, review the denial letter carefully to understand the reason. You may be able to appeal the decision or seek a revision if there’s new evidence.
- Revision Needed: Sometimes, additional information is required for a decision. Respond promptly to any requests for further information to facilitate the approval process.
Practical FAQ
What should I do if my prior authorization request is denied?
If your request is denied, follow these steps:
- Review the denial letter carefully for details on why your request was not approved.
- If you believe the denial was incorrect, check if you are eligible to appeal the decision. Most health plans, including United Healthcare, allow for an appeal process.
- Prepare any additional documentation that might support your appeal. This could include more detailed clinical information, a second opinion, or other relevant evidence.
- Submit an appeal to United Healthcare by following the instructions provided in the denial letter. Include your complete contact information and a clear explanation of why you believe the denial was incorrect.
- Keep a copy of all documents submitted with your appeal for your records.
If you still face difficulties, consider consulting with your healthcare provider for guidance on how to navigate the appeal process.
Tips, Best Practices, and How-To Information
Here are some additional tips to ensure you navigate the United Healthcare prior authorization process smoothly:
- Be Proactive: Initiate the prior authorization process as early as possible. Many services require several weeks for approval, so early action can prevent delays in treatment.
- Double-Check Information: Before submitting your form, double-check all entered information for accuracy. Even small errors can lead to processing delays.
- Communicate with Your Provider: Keep your healthcare provider in the loop about your prior authorization status. They can also provide any necessary support or additional information on your behalf.
- Utilize Online Resources: Take advantage of United Healthcare’s online tools for tracking your request and accessing forms. This can make the process more efficient and transparent.
- Understand Your Plan’s Requirements: Different health plans have different requirements for prior authorization. Familiarize yourself with the specific requirements for your plan to ensure compliance.
By following this detailed guide, you’ll be well-equipped to manage the United Healthcare prior authorization process effectively, ensuring that you get the care you need without unnecessary delays.
Remember, understanding and navigating prior authorization is not just about following procedures; it’s about ensuring you receive the best possible care for your health needs. With this guide, you’re now better prepared to handle the process confidently and efficiently.