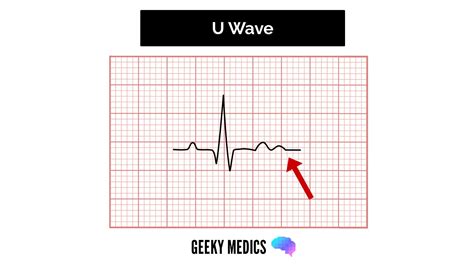
The U wave on an electrocardiogram (ECG) has long intrigued and perplexed medical professionals due to its elusive nature and unclear clinical significance. Often overshadowed by its more prominent neighbors—the P, QRS, and T waves—the U wave remains a subject of considerable debate and scrutiny. This comprehensive exploration aims to demystify the U wave, offering a blend of practical insights, evidence-based statements, and real-world examples to provide a clear understanding of this enigmatic component of the ECG.
To understand the U wave, we must first acknowledge its primary insight: its presence is often associated with hypokalemia (low potassium levels). This technical consideration holds significant application, as hypokalemia is a common electrolyte disorder that can lead to various cardiac complications if not addressed promptly. The actionable recommendation here is to monitor potassium levels in patients displaying a prominent U wave, especially in the context of cardiac arrhythmias or symptoms suggestive of electrolyte imbalance.
Key Insights
- Primary insight with practical relevance: U wave association with hypokalemia.
- Technical consideration with clear application: ECG showing U wave indicates the need to check potassium levels.
- Actionable recommendation: Monitor potassium levels in patients with U wave on their ECG.
The U wave’s genesis lies in late-phase cellular repolarization, occurring after the T wave. It is most frequently observed in leads V1 through V4. The presence of the U wave is usually subtle, but it becomes more pronounced with electrolyte imbalances, particularly hypokalemia. This phenomenon is well-documented and supported by numerous clinical studies which illustrate the wave’s prominence as a potassium level marker.
Another critical aspect to consider is the U wave’s correlation with certain cardiac conditions. Specifically, it can be seen in the context of digitalis toxicity, where the presence of the U wave may indicate the need for monitoring and potential dosage adjustment. This technical consideration underscores the necessity for a comprehensive approach when evaluating an ECG, ensuring no component—including the U wave—is overlooked.
Understanding the U wave’s clinical significance is paramount for accurate diagnosis and effective treatment planning. In practical terms, recognizing the U wave in an ECG should prompt an investigation into possible underlying electrolyte disturbances, particularly hypokalemia. This proactive approach can prevent the progression of potential cardiac issues, emphasizing the importance of a thorough and meticulous interpretation of the ECG.
What conditions can cause a U wave on an ECG?
The U wave is commonly associated with hypokalemia, but can also be seen in digitalis toxicity and certain other cardiac conditions.
How should one interpret a U wave on an ECG?
A U wave on an ECG should lead to an investigation into potassium levels, as it often indicates hypokalemia. Additionally, it should prompt a review for other potential conditions such as digitalis toxicity.
In summary, while the U wave may seem like a minor element of the ECG, it carries significant diagnostic and clinical implications. From its association with hypokalemia to its potential role in indicating digitalis toxicity, the U wave provides valuable insights when interpreted correctly. By emphasizing its importance and integrating it into routine ECG analysis, medical professionals can enhance patient care and ensure timely interventions for underlying conditions. This focused examination of the U wave serves as a crucial tool for the astute clinician, unraveling its mysteries to foster better patient outcomes.