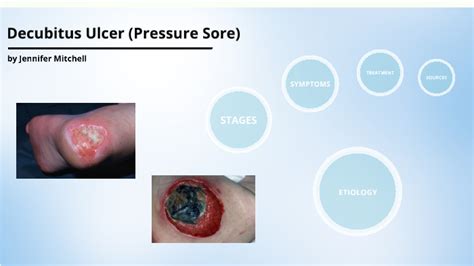
Decubitus ulcers, also known as pressure sores or bedsores, are a significant concern for individuals who are bedridden or have limited mobility. Specifically, sacrococcygeal decubitus ulcers, which occur around the tailbone, can be particularly painful and lead to serious complications if not addressed promptly. This guide aims to arm caregivers with the knowledge and practical strategies necessary to prevent these ulcers, ensuring comfort and promoting healing for those in their care.
The goal is to not just avoid these sores but to proactively engage in preventive measures that mitigate the risk of development, reduce discomfort, and encourage overall well-being. Let's dive into actionable strategies and practical tips to safeguard against this often preventable condition.
Understanding Sacrococcygeal Decubitus Ulcers
Sacrococcygeal decubitus ulcers develop when prolonged pressure restricts blood flow to the skin and underlying tissues around the tailbone. This restricted blood flow leads to tissue damage and, if not addressed, can progress to deeper ulcer formation. The primary risk factors include immobility, poor nutrition, friction, and shear force. As a caregiver, understanding these risk factors is crucial for implementing effective prevention strategies.
Immediate Actions to Prevent Sacrococcygeal Decubitus Ulcers
Taking immediate action is key to preventing pressure ulcers. Here are three critical steps to start with:
- Repositioning: Move the patient every two hours to relieve pressure on the sacrococcygeal area. Use pillows or specialized support cushions to distribute weight more evenly.
- Cleanliness: Keep the skin clean and dry. Use mild, fragrance-free soap and water, and gently pat the skin dry to prevent moisture-related damage.
- Diet: Ensure the patient receives a balanced diet rich in protein, vitamins, and minerals, which are essential for skin repair and overall health.
Detailed How-To: Comprehensive Repositioning Techniques
Repositioning is one of the most effective strategies in preventing decubitus ulcers. Here’s a detailed guide to help you ensure thorough and safe repositioning:
Step 1: Assess the Need
Determine how often the patient needs to be repositioned based on their level of mobility. Use a repositioning schedule to ensure no part of the body stays in one position for too long. Patients with limited mobility may need to be turned every one to two hours.
Step 2: Preparation
Gather necessary tools: pillows, transfer belts, and repositioning aids. Ensure the patient is comfortable and free from any immediate discomfort or pain.
Step 3: Rolling Technique
When repositioning a patient, use a rolling technique. Gently lift the patient by their shoulders and hips, rolling them onto their side. Ensure that the body moves as one unit to prevent shear force. Use pillows or specialized cushions to keep the body aligned and relieve pressure points.
Step 4: Positioning
For the sacrum and coccyx area, position the patient so that their buttocks are off the edge of the mattress, creating a gap to relieve pressure. Use cushions to create a gap between the bed and the patient’s tailbone.
Step 5: Document
Keep a log of repositioning times and any observations related to skin integrity. This documentation helps in creating a more tailored care plan and can identify any emerging issues early on.
Detailed How-To: Proper Skin Care Routine
A thorough skin care routine is essential to prevent moisture buildup, which can lead to skin breakdown. Here’s how to implement an effective skin care routine:
Step 1: Daily Inspection
Perform a daily skin inspection, paying special attention to the sacrococcgeal area. Look for signs of redness, swelling, or any breaks in the skin. Early detection can prevent the development of ulcers.
Step 2: Cleaning
When assisting with hygiene, ensure that the skin is cleaned gently and thoroughly. Use mild, non-alkaline soap and water, and avoid products with alcohol or fragrances, which can dry out the skin.
Step 3: Drying
After cleaning, pat the skin dry gently using a clean, soft towel. Avoid rubbing, which can cause friction. For areas that remain moist, use a moisture-absorbing powder or barrier creams to keep the skin dry.
Step 4: Dressing
Dress the patient in breathable fabrics like cotton. Avoid tight clothing that can cause friction or chafing. Regularly check that clothing fits well and doesn’t rub against pressure areas.
Step 5: Skin Protection
Apply barrier creams or lotions to areas prone to moisture buildup, especially under the patient’s legs, around the sacrum, and coccyx. These products help protect the skin from moisture and friction.
Detailed How-To: Nutritional Strategies
Good nutrition plays a vital role in maintaining skin integrity and preventing ulcers. Here’s how to support the patient’s nutritional needs:
Step 1: Dietary Assessment
Consult with a dietitian to assess the patient’s dietary needs and ensure they are receiving adequate protein, vitamins (particularly vitamin C and zinc), and minerals (like iron and calcium).
Step 2: Balanced Meals
Provide meals that include a variety of protein-rich foods, fresh fruits and vegetables, whole grains, and healthy fats. Encourage the patient to eat small, frequent meals if they have difficulty consuming large quantities.
Step 3: Hydration
Ensure the patient stays hydrated. Offer water regularly and consider adding hydrating foods like cucumbers and watermelon to their diet.
Step 4: Monitoring
Monitor the patient’s weight and any changes in their skin condition. Adjust the diet as necessary and report any significant changes to the healthcare team.
Practical FAQ: Common Questions from Caregivers
What are the signs of early decubitus ulcer development?
Early signs include persistent redness, warmth, swelling, or warmth around the sacrococcgeal area, as well as any areas where the skin appears pale or bluish. Patients might also experience pain or tenderness in these regions. If you notice any of these signs, it’s important to act immediately to prevent further development.
How often should patients be repositioned to prevent pressure ulcers?
Patients should generally be repositioned every one to two hours to relieve pressure and prevent the development of pressure ulcers. However, this frequency might need to be adjusted based on the patient’s level of mobility and the presence of risk factors.
What should caregivers do if a decubitus ulcer starts to develop?
If a decubitus ulcer starts to develop, it’s crucial to stop any activities that may have contributed to its formation. Reposition the patient immediately to relieve pressure on the affected area. Clean the ulcer gently with mild soap and water, and apply appropriate dressings as recommended by a healthcare professional. Monitor the ulcer closely and report any changes to the healthcare team promptly. In some cases, professional wound care may be required.
In conclusion, preventing sacrococcygeal decubitus ulcers involves a multifaceted approach, including regular repositioning, diligent skin care, and ensuring adequate nutrition. By implementing these strategies consistently and monitoring the patient’s condition closely, caregivers can significantly reduce the risk of developing pressure ulcers, ensuring greater comfort and improved quality of life for those in their care.