Nephrotic and nephritic syndromes are two distinct clinical entities that both arise from underlying kidney dysfunction. Understanding the precise differences between these conditions is essential for accurate diagnosis and effective management. This article delves into the essential distinctions, supported by practical insights and real-world examples.
Key Insights
- Primary insight with practical relevance: Despite their similar names, nephrotic and nephritic syndromes represent fundamentally different clinical presentations and etiologies.
- Technical consideration with clear application: Identifying whether a patient has nephrotic or nephritic syndrome helps in determining the underlying cause, thus guiding the appropriate therapeutic approach.
- Actionable recommendation: A thorough clinical evaluation, including urine analysis and serum tests, is crucial in differentiating these syndromes.
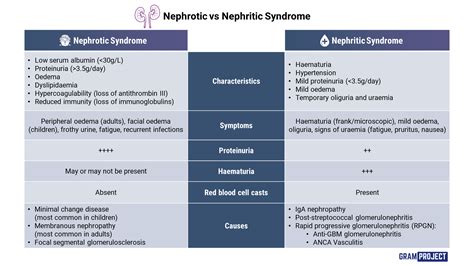
Defining Nephrotic Syndrome
Nephrotic syndrome is characterized by significant proteinuria, hypoalbuminemia, hyperlipidemia, and edema. This condition results from increased permeability of the glomerular filtration barrier, allowing significant amounts of protein to spill into the urine.For instance, a patient presenting with frothy urine and generalized swelling is likely experiencing nephrotic syndrome. The primary causes include minimal change disease, focal segmental glomerulosclerosis, and membranous nephropathy. Management typically focuses on controlling proteinuria with drugs such as corticosteroids and immunosuppressants, as well as addressing underlying diseases like diabetes or lupus.
Understanding Nephritic Syndrome
Conversely, nephritic syndrome is marked by hematuria, red blood cell casts, hypertension, and varying degrees of renal insufficiency. This syndrome involves inflammation and damage to the glomeruli, often leading to an active urine sediment.A practical example is a patient with acute post-infectious glomerulonephritis following streptococcal infection. Here, the kidney damage triggers inflammation, resulting in blood in the urine, swelling around the eyes, and elevated blood pressure. Management includes controlling blood pressure, anti-inflammatory treatment, and addressing the infectious source if applicable.
FAQ Section
Can nephrotic syndrome lead to nephritic syndrome?
While nephrotic and nephritic syndromes are distinct conditions, the underlying kidney disease causing nephrotic syndrome could progress to nephritic syndrome if not properly managed.
How do treatments differ between nephrotic and nephritic syndromes?
Treatment for nephrotic syndrome often involves corticosteroids and immunosuppressants to reduce proteinuria, while nephritic syndrome may require antihypertensives, anti-inflammatory medications, and sometimes antibiotics if an infection is present.
This article underscores the importance of differentiating between nephrotic and nephritic syndromes to deliver targeted and effective clinical care. By adhering to evidence-based guidelines and employing a precise diagnostic approach, healthcare professionals can better manage these complex conditions and improve patient outcomes.